Borderline personality disorder: definition, types, symptoms, causes, and treatments
Table of content
- What is borderline personality disorder (BPD)?
- What are the types of borderline personality disorder?
- What are the symptoms of borderline personality disorder?
- What are the causes of borderline personality disorder?
- What are the treatments for borderline personality disorder?
- What is the difference between borderline personality disorder and schizophrenia?

Borderline personality disorder (BPD) is a cluster B personality disorder indicated by the inability to control emotions, leading to dramatic and intense behaviors. Difficulties in regulating emotions often result in mood swings, fear of abandonment, and self-destructive tendencies.
The types of borderline personality disorder include discouraged borderline personality disorder, impulsive borderline personality disorder, petulant borderline, and self-destructive borderline.
Symptoms of BPD include a severe fear of being abandoned, frequently unstable, intense relationships, self-identity and self-image changes quickly, stress-related paranoia and periods of losing touch with reality, and risky and impulsive behavior.
The causes of BPD are genetic factors and brain abnormalities.
Treatment options for borderline personality disorder include dialectical behavior therapy (DBT), mentalization-based therapy (MBT), transference-focused psychotherapy (TFP), schema therapy (ST), and medication.
What is borderline personality disorder (BPD)?
Borderline personality disorder (BPD) is a mental health condition characterized by the inability to regulate emotions, resulting in unpredictable and severe mood cycles. Individuals with BPD often experience instability in relationships, struggling with fears of abandonment and shifting perceptions of others.
Maintaining consistent relationships with friends, family, or companions is often difficult due to the intense and overwhelming nature of emotional reactions. Impulsive behaviors, such as reckless spending or self-harm, frequently arise as a way to cope with distressing emotions.
Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) by the American Psychiatric Association categorizes BPD among cluster B personality disorders. As a cluster B personality disorder, the condition involves erratic and dramatic behaviors.
How common is borderline personality disorder?
Borderline personality disorder is relatively uncommon. According to the publication, “Borderline Personality Disorder” by Chapman et al., last updated in April 2024, the prevalence of BPD in the general population is estimated to be between 0.7% and 2.7% by nationwide epidemiologic studies, with symptoms typically presenting in early adulthood.
The rate of prevalence is 6% in primary care, 11% to 12% in outpatient psychiatric clinics, and 22% for psychiatric inpatients. While women have a slightly higher rate of BPD than men (3% versus 2.4%), women have a higher rate of BPD in outpatient psychiatric settings (78% versus 28%).
Reliable worldwide prevalence data for BPD in children are rare since historically BPD has been hardly diagnosed until adolescence. Limited research points to a modest but non-negligible rate even in late childhood.
For instance, according to a 2011 study by Zanarini et al., titled “Prevalence of DSM-IV Borderline Personality Disorder in Two Community Samples: 6,330 English 11-year Olds and 34,653 American Adults,” 3.2% of children aged 11 satisfied the DSM-IV criteria for BPD.
An estimated 3% of teenagers in the general population are thought to have BPD, according to a 2018 review by Guilé et al., titled “Borderline personality disorder in adolescents: prevalence, diagnosis, and treatment strategies”.
Finally, a 2021 paper by Botter et al., titled “Impact of borderline personality disorder traits on the association between age and health-related quality of life: A cohort study in the general population” reported a 3.2% prevalence of BPD in adults older than 55 years, with a decreasing trend due to factors like risky behavior and suicide.
What are the types of borderline personality disorder?
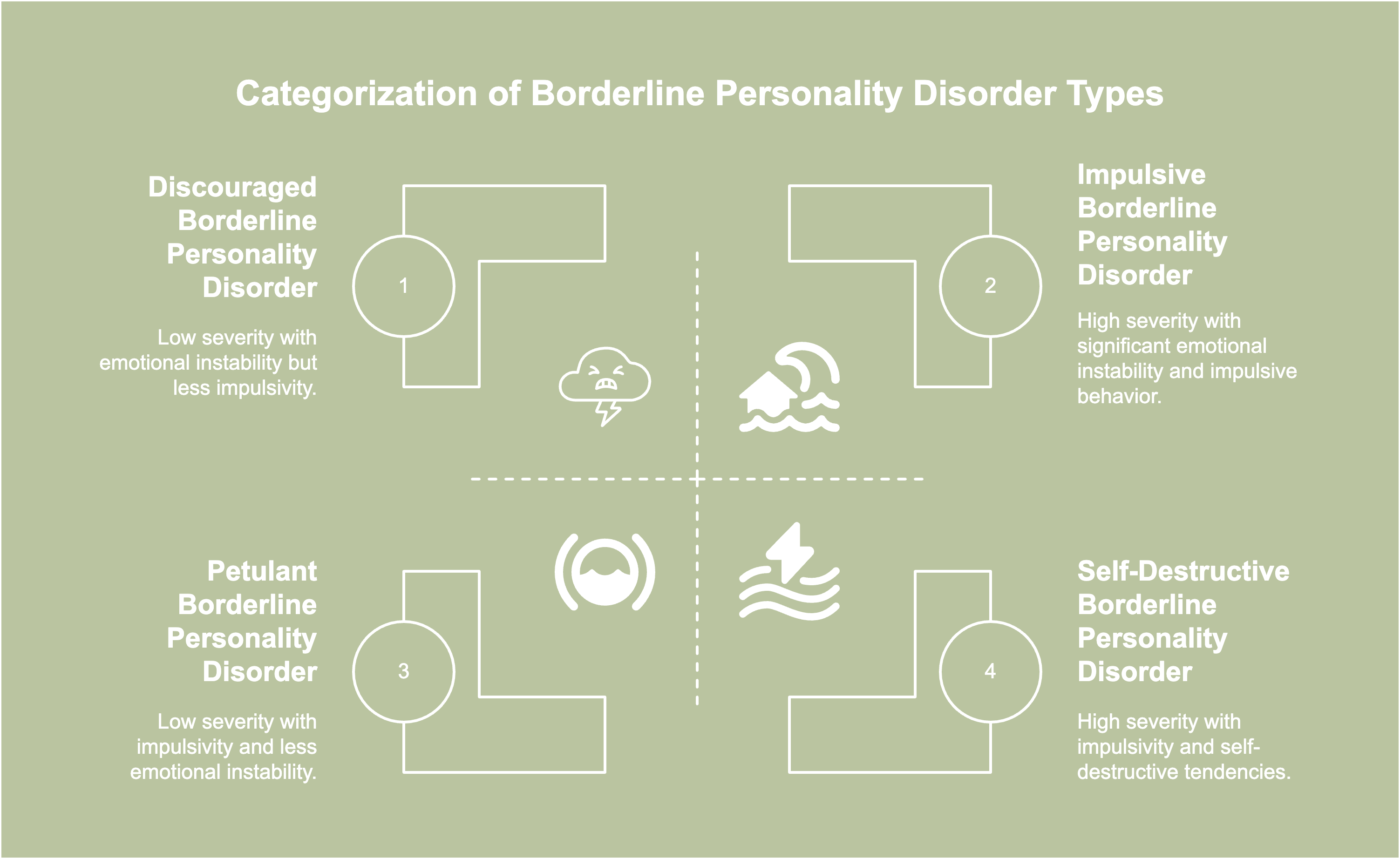
Types of borderline personality disorder often present with varying degrees of severity. The types of borderline personality disorder are listed below.
- Discouraged borderline personality disorder
- Impulsive borderline personality disorder
- Petulant borderline
- Self-destructive borderline
1. Discouraged borderline personality disorder
Discouraged borderline personality disorder, otherwise known as high-functioning or quiet BPD, is a subtype characterized by feelings of loneliness, low self-worth, and deep fear of abandonment, often leading to a submissive or people-pleasing demeanor.
Unlike the more outwardly intense forms of BPD, individuals with discouraged BPD internalize distress, making symptoms less visible to others. Many appear high-functioning in daily life but struggle with self-doubt and emotional suppression. A quiet sense of desperation often drives efforts to gain approval, creating cycles of dependency and resentment.
The discouraged subtype is defined by avoidant and dependent personality traits, alongside social withdrawal, guilt, self-doubt, and perfectionism, according to a 2022 paper by Duică et al., titled “Borderline Personality Disorder “Discouraged Type”: A Case Report.”
2. Impulsive borderline personality disorder
Impulsive borderline personality disorder is characterized by a pattern of high impulsivity, thrill-seeking tendency, and disregard for eventual consequences. Individuals with impulsive BPD often act on immediate urges, making decisions based on emotions rather than logic.
Engaging in risky behaviors, such as reckless driving, substance abuse, or unsafe sex, provides temporary relief but often leads to long-term consequences. Often, the need for stimulation and excitement takes precedence over worries about stability or safety.
Self-destructive tendencies in impulsive borderline personality disorder emerge when frustration or boredom becomes overwhelming, resulting in actions like self-harm or financial recklessness. The inability to sustain steady relationships and rapid mood swings are two factors contributing to turbulent emotions.
3. Petulant borderline
Petulant borderline is a subtype characterized by irritability, lack of self-control, and persistent feelings of dissatisfaction often manifesting as sentiments of being unloved or unworthy.
Individuals with petulant borderline disorder frequently struggle with irritability, reacting angrily or withdrawing when expectations are not met. A deep fear of abandonment fuels resentment, causing emotional outbursts or passive-aggressive behavior toward loved ones.
Sudden mood swings make relationships difficult, as frustration and insecurity often lead to unpredictable reactions. Feeling unworthy of care or attention often results in behavioral outbursts, pushing others away despite a strong need for validation.
4. Self-destructive borderline
Self-destructive borderline manifests through chronic self-sabotage, reckless decision-making, and a deep sense of hopelessness. A strong tendency toward self-punishment leads to actions like self-harm, substance abuse, or reckless relationships.
Intense emotional pain fuels destructive impulses, creating a cycle of suffering difficult to break. Feelings of worthlessness and guilt in people with self-destructive borderline disorder contribute to behaviors undermining personal well-being, often pushing away people trying to help.
What are the symptoms of borderline personality disorder?

Symptoms of borderline personality disorder are the patterns of thought, feeling, and action defining the condition. The symptoms of borderline personality disorder are listed below.
- A severe fear of being abandoned
- Frequently unstable, intense relationships
- Self-identity and self-image changes quickly
- Stress-related paranoia and periods of losing touch with reality
- Risky and impulsive behavior
1. A severe fear of being abandoned
A severe fear of being abandoned creates intense anxiety about losing relationships, whether real or perceived. Individuals with BPD often go to extreme lengths to prevent rejection, even when no actual threat exists.
Fear of abandonment leads to clingy behavior, frequent reassurance-seeking, or attempts to control relationships. When separation feels imminent, emotional reactions become overwhelming, resulting in panic, anger, or deep despair.
A 2018 paper by Palihawadana et al., titled “Reviewing the clinical significance of ‘fear of abandonment’ in borderline personality disorder” used the fictionalized clinical case of Sally, a bank executive with BPD, to illustrate the manifestations of abandonment fears: While at work, Sally can’t stop phoning Tom, her fiancé.
Sally is so distraught, she storms to Tom’s office and accuses him of abandoning her when he silences his phone during a meeting. As a means of coping with emotional distress, she contemplates self-harm.
Such a reaction pattern demonstrates how BPD sufferers’ frantic attempts to preserve relationships—even in a dysfunctional way—are a result of their fear of abandonment.
2. Frequently unstable, intense relationships
Unstable and intense relationships are a defining feature of BPD, often marked by rapid emotional shifts and deep insecurity. A strong desire for connection clashes with an overwhelming fear of rejection, making consistency in relationships difficult.
Feelings toward loved ones shift suddenly, moving from idealization to resentment with little warning. Even minor disagreements feel like betrayals, triggering anger, panic, or withdrawal. Affected individuals desperately try to prevent abandonment by becoming clingy or controlling, while others push people away first to avoid rejection.
Interpersonal hypersensitivity, resulting in drastic changes in relationships, is one of the hallmarks of borderline personality disorder, as noted in a 2022 article by Jeong et al., titled “Understanding a Mutually Destructive Relationship Between Individuals With Borderline Personality Disorder and Their Favorite Person.”
Individuals with BPD exhibit “splitting,” a psychological defense mechanism identified as perceiving a favorite person (FP) as wholly good (idealization) or completely bad (devaluation).
3. Self-identity and self-image changes quickly
A shifting self-identity and self-image lead to confusion about personal values, goals, and identity. Otherwise known as identity disturbance, the symptom causes individuals to struggle with a stable sense of self, often feeling unsure of who they are.
Rapid changes in interests, ambitions, and even moral beliefs occur, making consistency difficult. One day, a person feels confident and driven, while the next, deep self-doubt or hopelessness is the prevailing emotion. Self-perception dramatically shifts based on emotions, relationships, or external validation.
People with BPD struggle to define personal characteristics, maintain stable beliefs, and adapt to life transitions, according to a 2017 study by Natalie Gold and Michalis Kyratsous, titled “Self and identity in borderline personality disorder: Agency and mental time travel.”
Identity often shifts dramatically, leading to a fragmented sense of self and an “atemporal mode of existence,” where the perception of being the same person over time feels absent.
4. Stress-related paranoia and periods of losing touch with reality
Stress-related paranoia and brief episodes of losing touch with reality emerge in BPD due to heightened emotional sensitivity and fear of abandonment. Under extreme stress, perception of reality becomes distorted, leading to suspicion of others’ intentions.
Transient paranoia often arises in response to perceived rejection or betrayal, making trust difficult. Dissociation occurs, causing a sense of detachment from thoughts, emotions, or surroundings. Episodes of dissociation make the world feel unreal, as if everything is distant or dreamlike.
5. Risky and impulsive behavior
Risky and impulsive behavior stems from difficulty regulating emotions and seeking immediate relief from distress. Making decisions without taking long-term effects into account frequently results in behaviors like careless spending, risky sexual behavior, irresponsible driving, and drug usage.
Sudden urges drive behavior, creating a pattern of instability in daily life. Emotional pain or boredom pushes individuals toward thrill-seeking activities or dangerous situations. Feelings of emptiness often contribute to seeking excitement as a way to fill an emotional void.
Repeated engagement in self-destructive choices reinforces cycles of regret and further emotional distress.
How is borderline personality disorder diagnosed?
Borderline personality disorder is diagnosed by mental health professionals through a comprehensive psychological evaluation. Clinicians assess emotional instability, impulsive behaviors, self-image disturbances, and difficulties in relationships to determine if symptoms align with DSM-5 criteria.
The DSM-5 requires that at least five of the nine specified diagnostic criteria be met, including intense fear of abandonment, unstable relationships, identity disturbance, impulsivity, self-harming behaviors, emotional instability, chronic feelings of emptiness, intense anger, and transient stress-related paranoia or dissociation.
Further information into behavioral patterns is often gained through in-depth interviews, self-report assessments, and input from close family or friends. Differentiating BPD from other conditions with comparable symptoms, such bipolar disorder or complex post-traumatic stress disorder (PTSD), requires a comprehensive evaluation.
Symptoms must be persistent, affect multiple aspects of life, and result in substantial distress or impairment in daily functioning.
What are the causes of borderline personality disorder?
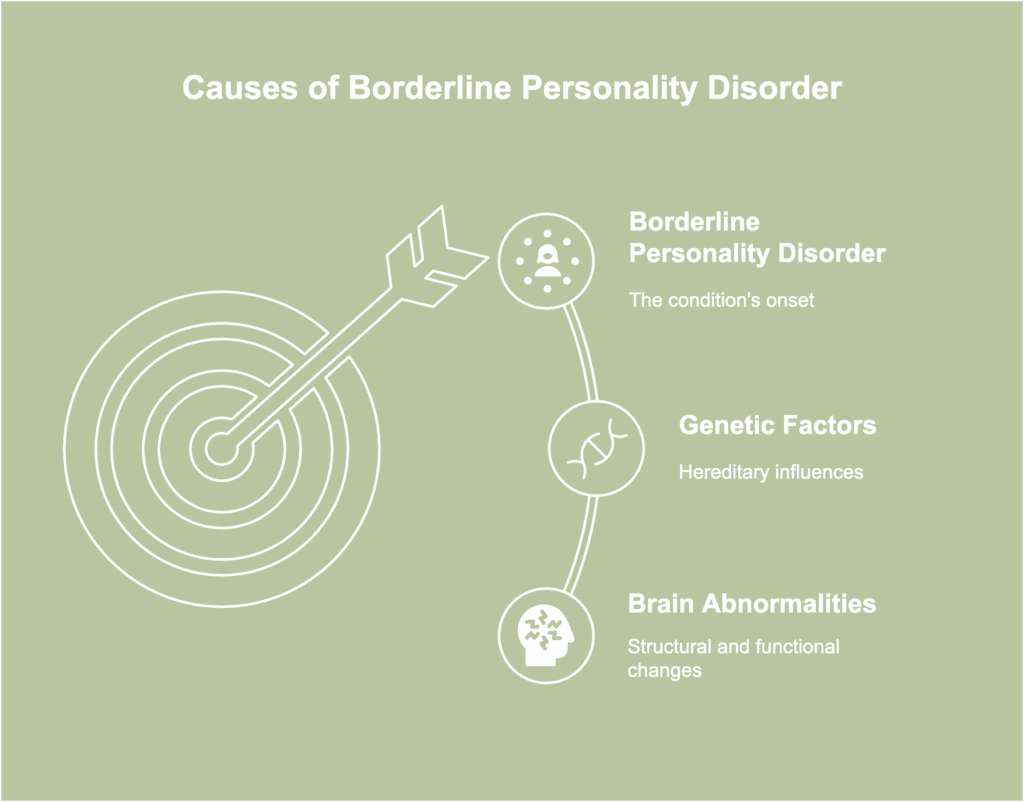
Causes of borderline personality disorder describe the primary reasons behind the condition’s onset. The causes of borderline personality disorder are listed below.
- Genetic factors
- Brain abnormalities
1. Genetic factors
Through raising susceptibility to emotional dysregulation and impulsive conduct, genetic factors cause BPD. People with a family history of borderline personality disorder or similar mental health issues are more vulnerable to developing the disorder.
According to a 2023 paper by Ansari et al., titled “Genetic Influences on Outcomes of Psychotherapy in Borderline Personality Disorder: A Narrative Review of Implications for Personalized Treatment,” genetic factors are responsible for approximately 40-60% of the variation in BPD, as demonstrated by twin studies conducted in a variety of countries.
Adverse environments, such as childhood trauma, neglect, or abusive family dynamics, amplify genetic inclinations toward impulsivity and emotional sensitivity.
2. Brain abnormalities
Brain abnormalities influence emotional regulation, impulse control, and stress reactions, therefore contributing to BPD. Development of symptoms depends much on structural and functional variations in the amygdala, prefrontal cortex, and hippocampus.
An overactive amygdala increases emotional sensitivity, fueling strong reactions to perceived dangers or stress. Lower activity in the prefrontal cortex weakens impulse control and decision-making, creating challenges in managing emotions efficiently.
Stronger stress reactions and difficulty distinguishing prior trauma from present circumstances are due to anomalies in the hippocampus, a brain region responsible for processing memory and emotional responses.
A study titled “Structural brain abnormalities in borderline personality disorder correlate with clinical severity and predict psychotherapy response” published in 2021 by Sampedro et al., verified the existence of structural abnormalities in patients with BPD, specifically a decrease in gray matter volume (GMV) in prefrontal cortex regions and an increase in GMV in limbic structures.
Such structural variations predicted how well patients respond to psychotherapy and were correlated with the severity of symptoms.
What are the risk factors for borderline personality disorder?

Risk factors for borderline personality disorder refer to conditions or experiences increasing the likelihood of developing the condition. The risk factors for borderline personality disorder are listed below.
- Abandonment as a child or teen: Losing a caregiver or experiencing inconsistent emotional availability fosters deep-seated fears of rejection. Early separation or neglect creates lasting insecurity, making relationships feel unstable or unreliable. Individuals often develop intense dependency or engage in self-sabotaging behaviors to prevent perceived abandonment.
- Early trauma and abuse: Exposure to physical, emotional, or sexual abuse during formative years disrupts emotional development. Trauma interferes with trust, leading to unstable relationships and intense fear of abandonment. Survivors often struggle with emotional regulation, increasing impulsivity and self-destructive tendencies. Repeated exposure to harm reinforces negative self-perception, further fueling BPD symptoms.
- Environmental factors: Bullying, dysfunctional households, and neglect are all closely linked to the emergence of BPD, as noted in a 2021 review by Bozzatello et al., titled “Borderline Personality Disorder: Risk Factors and Early Detection.” Traumatic experiences raise the risk of self-harming behaviors and other symptoms, as well as contributing to early-onset BPD. BPD symptoms are consistently predicted by a low socioeconomic background; research shows poverty necessitating public help predicts the emergence of BPD symptoms in adolescence. Inadequate parent-child boundaries (psychological control, guilt induction, and triangulation) and parental conflict additionally play a role in the development of BPD symptoms.
- Family-related factors: Low warmth and maternal satisfaction, hostility, rejection, severe discipline, broken communication, negative emotions, over-involvement, and inconsistency were identified as significant psychosocial risk factors for the development of BPD in studies, according to a 2021 paper by Bozzatello et al., titled “Borderline Personality Disorder: Risk Factors and Early Detection.” Conflict between mothers and children holds particular importance, with research suggesting a potential link to the development of BPD in adulthood. Children experiencing BPD symptoms are more likely to have overbearing and intrusive parents, particularly the mother, as well as low levels of warmth, affection, empathy, and connection.
- Temperamental traits: Individuals born with heightened emotional sensitivity struggle to regulate intense feelings. Extreme mood fluctuations make coping with stress and interpersonal challenges difficult. High reactivity to emotions increases impulsive decision-making, reinforcing unstable behaviors. A naturally sensitive temperament, when combined with an invalidating environment, increases the risk of developing BPD.
Who is affected by borderline personality disorder?
Individuals affected by borderline personality disorder include adolescents, adults, men, women, and people with a family history of mental health conditions. Symptoms often emerge during teenage years or early adulthood, with emotional instability, impulsivity, and difficulties in relationships becoming apparent.
A persistent fear of abandonment influences behavior, leading to clinginess, extreme reactions to perceived rejection, or self-sabotaging tendencies in relationships. Although females receive diagnoses more frequently, males experience the disorder as well, sometimes displaying symptoms through aggression or substance use.
Individuals who have endured childhood trauma, neglect, or abandonment face a heightened risk, as early adverse experiences contribute to emotional dysregulation. Genetics play a role too—increasing susceptibility in those with relatives diagnosed with BPD or similar conditions.
Can borderline personality disorder be prevented?
No, borderline personality disorder cannot be prevented. There is no known way to eliminate the risk of developing BPD, as genetic, neurological, and environmental factors contribute to its onset.
However, early intervention and emotional support during childhood reduce the likelihood of severe symptoms later in life. Individuals’ susceptibility to emotional dysregulation is diminished by the establishment of effective coping mechanisms in a stable and supportive environment.
Therapy for children and adolescents displaying early signs of emotional instability promotes better self-regulation and resilience. Managing stress, fostering secure attachments, and addressing traumatic experiences early decrease the disorder’s impact.
Although prevention is not guaranteed, identifying and treating risk factors early improves overall emotional well-being. A proactive approach to mental health care offers the best chance of mitigating long-term difficulties associated with BPD.
What are the treatments for borderline personality disorder?

Treatments for borderline personality disorder denote therapeutic strategies aimed at alleviating symptoms and enhancing emotional stability. The treatments for borderline personality disorder are listed below.
- Dialectical behavior therapy (DBT): For the purpose of helping people deal with strong emotions, DBT promotes emotional regulation, distress tolerance, mindfulness, and interpersonal effectiveness. DBT lessens impulsivity and emotional instability by tackling self-destructive behaviors and developing coping mechanisms. DBT is a successful treatment for BPD, according to a 2024 systematic review by Hernandez-Bustamante et al., titled “Efficacy of Dialectical Behavior Therapy in the Treatment of Borderline Personality Disorder: A Systematic Review of Randomized Controlled Trials,” especially when it comes to lowering suicidality, depression, self-injury, and emotional dysregulation.
- Mentalization-based therapy (MBT): MBT enhances the ability to understand and interpret mental states of oneself and others. Strengthening mentalization skills reduces impulsive reactions and emotional outbursts by fostering a more reflective approach to interpersonal situations. Relationship stability, social awareness, and emotional control are the main goals of MBT, according to a 2024 report by Leichsenring et al., titled “Borderline personality disorder: a comprehensive review of diagnosis and clinical presentation, etiology, treatment, and current controversies.” Combining individual and group therapy, the approach works especially well for patients struggling with emotional dysregulation and attachment issues.
- Transference-focused psychotherapy (TFP): A form of psychodynamic therapy, TFP focuses on the patterns of emotional responses and relationship dynamics formed in early life. Through interactions with the therapist, individuals recognize and modify distorted perceptions of themselves and others. The process lessens severe mood swings, abandonment anxiety, and erratic self-perception.
- Schema therapy (ST): Schema therapy identifies and challenges deeply ingrained negative beliefs and maladaptive coping mechanisms developed during early experiences. Individuals acquire the ability to replace destructive thought patterns with healthier perspectives by addressing core emotional wounds. As perceptions of self and the world shift, emotional regulation improves, and a stronger sense of self-worth develops.
- Medication: No medications have been approved specifically for BPD, but pharmacotherapy is useful for treating comorbid conditions or managing acute symptoms. As explained by a 2024 review from Leichsenring et al., titled “Borderline personality disorder: a comprehensive review of diagnosis and clinical presentation, etiology, treatment, and current controversies,” medications for BPD include antidepressants, mood stabilizers, and antipsychotics. Treatment for mood disorders generally includes antidepressants, notably selective serotonin reuptake inhibitors (SSRIs). Mood stabilizers like valproate and lithium help certain patients become less impulsive and unstable. Antipsychotics like olanzapine and aripiprazole treat emotional instability and cognitive-perceptual problems. Crisis situations or serious comorbid conditions (such as depression or anxiety) warrant the use of medication for a brief period of time only.
What is the difference between borderline personality disorder and schizophrenia?
The difference between borderline personality disorder and schizophrenia is in the symptoms, causes, and overall effects on functioning associated with each condition. The differences between borderline personality disorder and schizophrenia are outlined in the table below.
| Difference Between Borderline Personality Disorder and Schizophrenia | ||
| Aspect | Borderline personality disorder | Schizophrenia |
| Core symptoms | Emotional instability, impulsivity, fear of abandonment, and unstable relationships | Delusions, hallucinations, disorganized thinking, negative symptoms (e.g., lack of motivation, reduced emotional expression). |
| Causes | Genetic factors and brain abnormalities | Genetic predisposition, neurodevelopmental abnormalities, and environmental stressors. |
| Reality perception | Transient paranoia or dissociation under stress | Persistent psychotic symptoms, including hallucinations and delusions |
| Insight | Partial insight; patients recognize emotional dysregulation but struggle to control it. | Poor insight is common, especially during acute psychotic episodes. |
| Interpersonal relationships | Intense and unstable; characterized by idealization and devaluation. | Generally impaired due to social withdrawal, disorganized thinking, or paranoia. |
| Impact on functioning | Struggles with emotional regulation and relationships | Severe impairment in daily functioning, often requiring long-term care |
| Treatment approaches | Primarily psychotherapy (e.g., DBT, MBT, ST) and limited medication use. | Antipsychotic medications as the primary treatment, with psychosocial interventions as supportive therapies. |
While both BPD and schizophrenia are serious mental health conditions, significant differences exist in symptoms, treatment approaches, and underlying causes. Accurate diagnosis and successful treatment planning remain reliant on being able to distinguish such distinctions.


