Opioid agonist therapy (methadone maintenance): definition, goal, how it works, and effectivity
Table of content
- What is opioid agonist therapy (methadone maintenance)?
- What is the goal of opioid agonist therapy?
- How does opioid agonist therapy work?
- How is opioid agonist therapy done?
- How long does opioid agonist therapy last?
- What are the benefits of opioid agonist therapy?
- What are the risks of opioid agonist therapy?
- Who supervises opioid agonist therapy?
- Is opioid agonist therapy effective?
- What is the difference between opioid agonist therapy and medication-assisted therapy?
- What is the difference between opioid agonist therapy and opioid replacement therapy?

Opioid agonist therapy (methadone maintenance) involves the long-term use of methadone to manage opioid dependence and reduce withdrawal symptoms. The treatment helps stabilize individuals by preventing cravings and blocking the effects of illicit opioids without producing intense euphoria.
The goal of opioid agonist therapy is to alleviate both the physical and mental distress associated with opioid dependence through the use of safer, more closely monitored drugs. With decreased cravings for illegal opioid usage and more treatment participation, the strategy promotes long-term recovery.
Opioid agonist therapy works by employing drugs to subtly activate opioid receptors without producing severe highs. Drugs with consistent effects, like buprenorphine or methadone, make detoxification less difficult.
Opioid agonist therapy is effective because it creates a steady chemical balance in the brain, allowing individuals to function without the instability from unmanaged opioid dependence.
What is opioid agonist therapy (methadone maintenance)?
Opioid agonist therapy (methadone maintenance) is a medically supervised treatment using methadone, a long-acting opioid agonist, to reduce cravings and ease withdrawal symptoms in individuals dependent on opioids.
Opioid addiction disrupts daily functioning and increases the likelihood of overdose, making consistent treatment essential for recovery.
Methadone maintenance allows individuals to regain stability, participate in counseling or rehabilitation programs, and improve overall quality of life.
What does opioid agonist mean?
Opioid agonist means a drug binding to and activating opioid receptors located in the brain and body. Opioid receptors support control of mood, pain, and numerous bodily functions. Stimulation of opioid receptors by an opioid agonist results in effects like pain relief, relaxation, and occasional euphoria.
Among opioid agonists used in medical treatment are morphine and methadone. The medicine plays the function of endorphins—naturally occurring substances controlling stress and pain. During addiction treatment, opioid agonists support relief from withdrawal symptoms and lower drug cravings.
Occupation of opioid receptors blocks the effects of more dangerous opioids like heroin. Although useful under medical supervision, opioid agonists cause dependence when misused.
What is the goal of opioid agonist therapy?

The goal of opioid agonist therapy is to stabilize brain chemistry, support long-term recovery, and lower the risk of relapse by providing a controlled, legal alternative to illicit opioids. Through employing agonist opioids like methadone, the method regulates the activation of opioid receptors.
People are able to function more normally as cravings and drug withdrawal symptoms become easier to control. The therapy reduces emotional and physical distress linked to addiction. Stabilization of brain chemistry supports clearer thinking and emotional regulation.
How does opioid agonist therapy work?
Opioid agonist therapy works by using medications steadily activating opioid receptors without causing intense euphoria. Controlled effects from medications like buprenorphine or methadone reduce the discomfort of detoxification and reduce cravings for opiate addiction.
Cognitive clarity and emotional regulation are enhanced through the process of restoring balance in brain chemistry. More stability generally enables people to resume regular activities and obligations. Disruptive tendencies associated with opioid dependence are reduced by the therapy.
How does methadone work in opioid agonist therapy?
Methadone works in opioid agonist therapy as a long-acting, synthetic opioid helping stabilize individuals with opioid dependence. The medication attaches to opioid receptors in the brain, producing mild effects while preventing extreme highs and crashes linked to stronger opioids.
Due to methadone’s long duration, a single dose offers effects lasting the entire day, lowering the need for repeated intake. According to a publication by Mehnoor Durrani and Kamna Bansal last updated in January 2024, titled “Methadone,” the United States Food and Drug Administration (FDA) has approved methadone to treat opioid use disorder in federally authorized opioid treatment facilities.
Prescriptions for methadone are used for both maintenance treatment and detoxification. Patients who receive long-term methadone treatment as opposed to short-term treatment show superior success in terms of opioid abstinence rates.
How is opioid agonist therapy done?
Opioid agonist therapy is done by having individuals visit a clinic or pharmacy daily for supervised medication distribution during the early stages, according to a 2022 paper by Russell et al., titled “Opioid agonist treatment take-home doses (‘carries’): Are current guidelines resulting in low treatment coverage among high-risk populations in Canada and the USA?.”
Daily oversight reduces risks like misuse or diversion and helps guarantee adherence. Usually, patients must provide regular urine samples—often weekly—to monitor for illicit drug use and confirm compliance with the prescribed opioid agonist therapy (OAT) regimen.
Medications like methadone or buprenorphine (Suboxone or Sublocade) are administered in OAT to help manage addiction to opioids. Suboxone contains buprenorphine, a partial opioid agonist, and naloxone, an opioid antagonist, helping prevent misuse of the medication.
Buprenorphine activates opioid receptors to lessen urges for drug use and discomfort from cessation while blocking the effects of illicit opioids. Naloxone is included to discourage misuse of Suboxone, counteracting any euphoric effects when the medication is abused.
Sublocade, an injectable form of buprenorphine, offers a monthly alternative to oral medications, providing a consistent dose without the need for daily taking. The treatment is provided under medical supervision to ensure the proper dosage and prevent complications. Patients start taking methadone, buprenorphine, or Suboxone after an initial detox period to avoid precipitating withdrawal symptoms.
How long does opioid agonist therapy last?
Opioid agonist therapy lasts at least one to two years for most individuals, though some remain in treatment for much longer, according to a 2016 publication titled “Opioid agonist therapy” from the Centre for Addiction and Mental Health (CAMH).
The duration depends on personal needs, progress in recovery, and clinical guidance, with long-term maintenance often recommended to support stability and prevent relapse. The initial phase often focuses on stabilization, where individuals start on a specific medication like methadone and gradually adjust the dose.
After stabilization, therapy keeps physical symptoms under control and decreases cravings for opioids. With time and medical supervision, gradual dose reduction becomes possible for certain individuals.
What are the benefits of opioid agonist therapy?
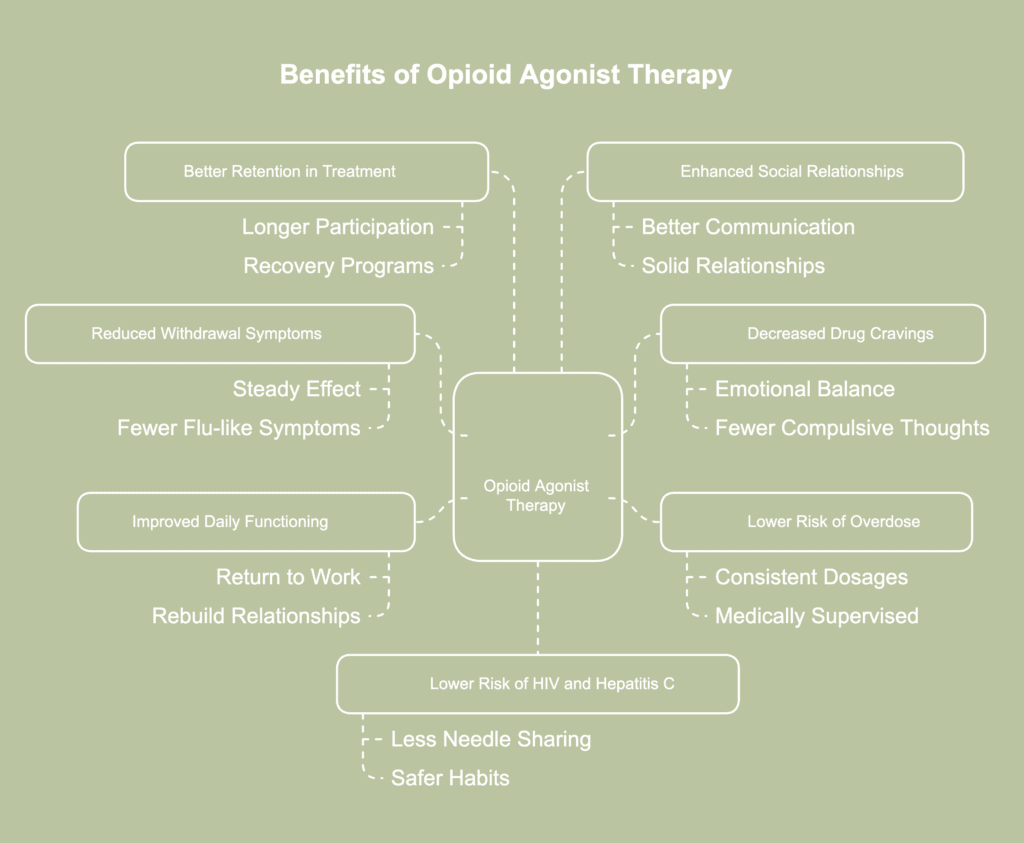
Benefits of opioid agonist therapy are the favorable results connected with treating opioid dependency by means of drugs such as methadone. The benefits of opioid agonist therapy are listed below.
- Reduced withdrawal symptoms: Opioid agonist therapy (OAT) eases physical discomfort linked to stopping opioid use. Medications such as methadone deliver a steady effect, preventing severe reactions during detoxification. Individuals feel more stable and notice fewer flu-like symptoms, chills, or muscle aches. Relief from such effects enables greater focus on recovery without being consumed by ongoing distress.
- Decreased drug cravings: OAT targets brain receptors to help minimize urges for opioid use. Less craving means reduced risk of returning to harmful substances. Individuals often achieve greater emotional balance and fewer compulsive thoughts about using drugs. Strengthening commitment to long-term recovery goals is achieved through managing cravings.
- Lower risk of overdose: Replacing illicit opioids with medically supervised alternatives, opioid agonist therapy helps prevent accidental overdoses. Medications provide consistent dosages, in contrast to illicit narcotics containing unpredictable and hazardous chemicals. With a greater relative effect (rate ratio of 4.80) than all-cause mortality (rate ratio of 3.20), methadone treatment significantly lowers overdose mortality, reflecting how the approach reduces illicit opioid use, according to a 2017 report by Sordo et al., titled “Mortality risk during and after opioid substitution treatment: systematic review and meta-analysis of cohort studies.”
- Improved daily functioning: Regular routines and improved physical health are a few of the benefits of OAT. Individuals are able to return to work, rebuild relationships, or pursue education. Productivity rises when one is able to control emotions and think clearly. Stability and confidence increase when structure is restored.
- Better retention in treatment: OAT encourages people to continue participating in recovery programs for a longer period of time.With a median retention period of 101 days, methadone patients showed better numerical retention than buprenorphine/naloxone patients, at 58 days, according to results from a 2022 study by Joseph Sadek & Joseph Saunders, titled “Treatment retention in opioid agonist therapy: comparison of methadone versus buprenorphine/naloxone by analysis of daily-witnessed dispensed medication in a Canadian Province.”
- Enhanced social relationships: Consistent recovery support allows individuals to rebuild trust with loved ones. Stability in emotions promotes better communication and more solid relationships. Relationships usually become better as detrimental habits decrease. Support from family is essential to sustaining success.
- Lower risk of human immunodeficiency virus (HIV) and Hepatitis C: Lessening the likelihood of needle sharing and illegal drug use, OAT helps minimize the transmission of infectious diseases. Through supervised care, individuals engage in fewer high-risk behaviors often associated with intravenous substance use. Access to hygienic materials and health risk education help further promote safer habits. Overall health increases and the risk of major health problems decreases as a result.
What are the risks of opioid agonist therapy?
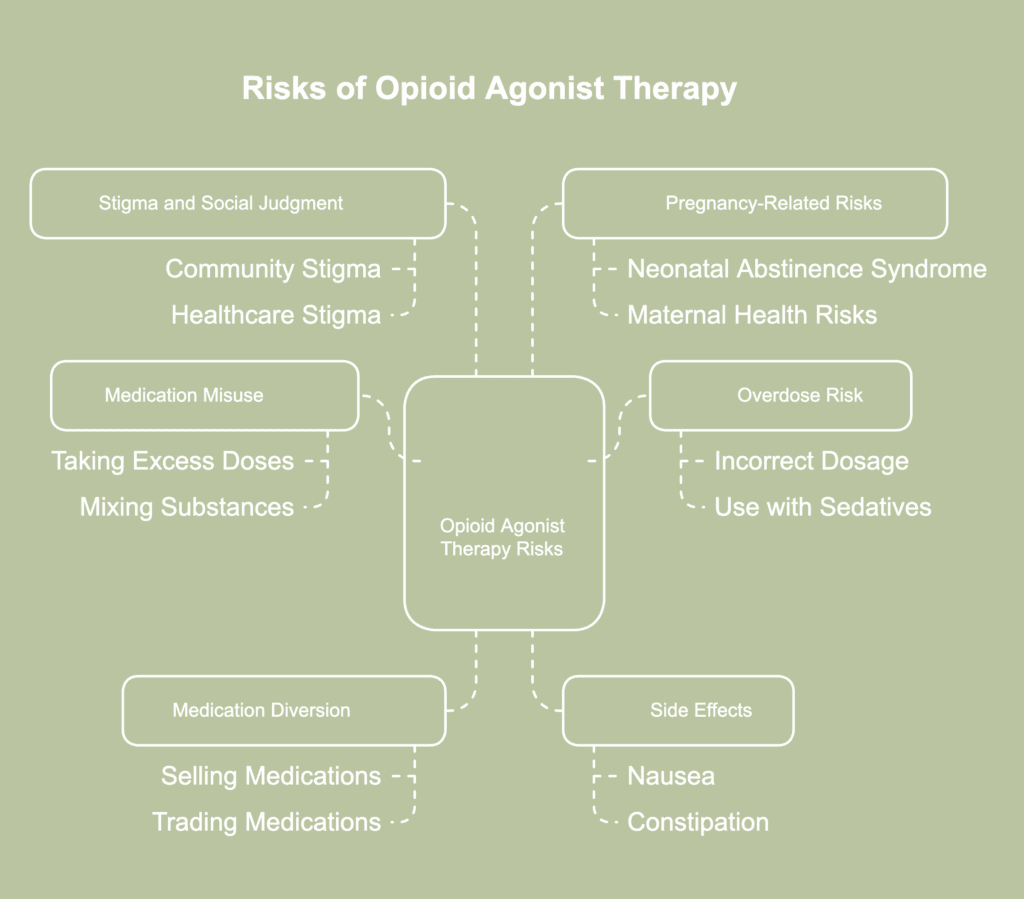
Risks of opioid agonist therapy refer to potential negative effects or complications arising during the use of medications such as methadone to manage opioid dependence. The risks of opioid agonist therapy are listed below.
- Potential for medication misuse: Although opioid agonist therapy (OAT) includes medical supervision, medications for OAT still carry a risk of misuse. Taking doses beyond medical recommendations or mixing substances often leads to harmful effects. Certain individuals attempt to inject or snort oral medications, raising the likelihood of severe complications. Preventing improper use involves ongoing monitoring, access to counseling, and thorough patient education.
- Risk of overdose: Overdose becomes a concern when medications are taken incorrectly or used alongside sedatives like benzodiazepines or alcohol. Methadone, in particular, builds up in the body over time, making miscalculation or double-dosing especially risky. Unsupervised or unmonitored use increases the danger of respiratory depression and other life-threatening reactions.
- Diversion of medication: Certain patients sell, trade, or distribute prescribed opioid agonists, fueling illegal drug circulation. Diversion weakens the structure of treatment programs and exposes others to potential misuse of the medication. Participants in a 2023 study by Evans et al., titled “Diversion of medications to treat opioid use disorder: Qualitative findings from formerly incarcerated adults in Massachusetts” reported drug diversion for therapeutic purposes (e.g., assisting individuals in withdrawal, particularly those not enrolled in the medications for opioid use disorder (MOUD) program owing to delayed or denied access), coercion, financial incentives, or personal dose preferences.
- Side effects: Medications used in OAT produce side effects like nausea, constipation, dry mouth, or drowsiness. Although symptoms often subside with continued use, certain individuals still experience discomfort interfering with daily functioning. More severe reactions, like breathing problems or heart rhythm disturbances, occur in rare cases. Regular check-ups ensure any complications are detected early and addressed promptly.
- Stigma and social judgment: Although medically accepted, opioid agonist therapy often faces stigma within communities and healthcare environments. Patients often feel judged or misunderstood, discouraging full participation in recovery. Stigmatizing views affect jobs, homes, and relationships, therefore adding more challenges to long-term growth. A more encouraging environment for people in treatment is contingent upon awareness and education.
- Pregnancy-related risks: Pregnant individuals using OAT must follow carefully adjusted treatment plans to protect both maternal and fetal health. Methadone or other medications lead to neonatal abstinence syndrome (NAS), where newborns experience withdrawal after birth. While OAT is often safer than continued illicit opioid use during pregnancy, the approach requires close medical supervision. Prenatal care tailored to OAT ensures better outcomes for both parent and child.
Who supervises opioid agonist therapy?
Opioid agonist therapy is supervised by licensed healthcare professionals trained in addiction medicine, such as physicians, nurses, pharmacists, counselors, and social workers. The evaluation of patient requirements, prescription of medications such as methadone or Suboxone, and the monitoring of progress are all responsibilities of physicians.
Nurses assist with daily medication administration, track physical responses, and report any adverse effects. Pharmacists ensure correct dispensing, manage dosages, and educate patients on safe medication use. Counselors give behavioral support, therefore enabling people to develop coping mechanisms and stay dedicated to treatment goals.
Social workers often coordinate care plans, connecting patients to housing, employment, or community support. Clinical teams work together to evaluate effectiveness and adjust treatment strategies as necessary.
Is opioid agonist therapy effective?
Yes, opioid agonist therapy is effective. The approach significantly lowers the risk of relapse by stabilizing brain chemistry and curbing the intense need for opioids. Better participation in rehabilitation programs and more consistent development are both made possible by the therapy’s structured nature.
The evidence supporting opioid agonist therapy (OAT) as a highly effective, evidence-based treatment for opioid use disorder (OUD) was further substantiated by a 2016 publication by Sarah E. Wakeman, titled “Using Science to Battle Stigma in Addressing the Opioid Epidemic: Opioid Agonist Therapy Saves Lives.” It claimed that agonist therapy achieves high retention rates (60%–80%), significantly reduces illicit opioid use (to 15% among treated individuals), and reduces relapse rates by 50% compared to behavioral interventions.
Additionally, OAT is cost-effective, with the ability to save $1.80 for every dollar spent and a 50 – 62% reduction in healthcare costs—possibly leading to significant savings for society.
What is the difference between opioid agonist therapy and medication-assisted therapy?
The difference between opioid agonist therapy and medication-assisted therapy describes how one technique to treating opioid use disorder differs from another. The differences between opioid agonist therapy and medication-assisted therapy are detailed in the table below.
| Difference Between Opioid Agonist Therapy and Medication-Assisted Therapy | ||
| Aspect | Opioid agonist therapy (OAT) | Medication-assisted therapy (MAT) |
| Definition | A treatment using opioid medications activating opioid receptors | A comprehensive approach combining medications with counseling or therapy |
| Scope of medication | Focuses mainly on methadone and buprenorphine | Includes methadone, buprenorphine, and opioid antagonists like naltrexone |
| Goal | Reduces withdrawal symptoms and stabilizes opioid-dependent individuals | Aims to treat addiction using medical and psychological support together |
| Medication type | Uses opioid agonists mimicking the effects of opioids | Involves agonists, partial agonists, or antagonists |
| Behavioral component | May or may not include counseling | Always includes counseling or behavioral therapy |
| Application | Primarily for opioid use disorder | Used for opioid, alcohol, or other substance use disorders |
The management of substance use disorders is greatly aided by both treatments. Medication-assisted therapy, however, presents a more inclusive method addressing behavioral as well as physical components of recovery.
What is the difference between opioid agonist therapy and opioid replacement therapy?
The difference between opioid agonist therapy and opioid replacement therapy emphasizes how two nearly comparable strategies differ in focus and intent. The differences between opioid agonist therapy and opioid replacement therapy are specified below.
| Difference Between Opioid Agonist Therapy and Opioid Replacement Therapy | ||
| Aspect | Opioid agonist therapy (OAT) | Opioid replacement therapy (ORT) |
| Definition | A subset of ORT; uses drugs activating opioid receptors | A broad treatment approach involving the substitution of safer opioids |
| Primary goal | Manage withdrawal and cravings through receptor activation | In addition to basic withdrawal and craving management, ORT prevents relapse and supports either stabilization or abstinence |
| Medications used | Uses only opioid agonists such as methadone and buprenorphine | Includes opioid agonists (e.g., methadone, buprenorphine) and antagonists (e.g., naltrexone) |
| Goal | Stabilizes neurochemistry and reduces withdrawal and cravings | Reduces harm from illegal drug use and lowers the risk of overdose or infection |
| Treatment flexibility | Focused specifically on agonist-based stabilization | Offers more varied options for individualized care |
Opioid replacement therapy serves as a comprehensive strategy including various medication options to support recovery from opioid dependence. Within the approach, opioid agonist therapy plays a more specific role focused on stabilizing brain chemistry and reducing cravings through controlled use of opioid-based medications.


