Comorbidities with substance use disorders: definition, effects, symptoms, and treatment
Table of content
- What does comorbidity with substance use disorders mean?
- What are the most common comorbidities with substance use disorders?
- How common are comorbidities in substance use disorders?
- What is the difference between dual diagnosis and comorbidity with substance use disorder?
- Why do mental disorders and substance use disorders occur together?
- What are the effects of comorbid conditions in substance use disorders?
- What are the symptoms of comorbidities with substance use disorders?
- What are the risk factors for comorbidities with substance use disorders?
- How are comorbidities with substance use disorders diagnosed?
- How are comorbidities with substance use disorders treated?

Comorbidity with substance use disorders means the simultaneous presence of a medical condition alongside an addiction problem in the same individual.
The effects of comorbid conditions in substance use disorders include increased severity of symptoms compared to what is typically exhibited when either disorder occurs alone; exacerbation of mental health disorder symptoms due to drug use; and aggravation of psychological symptoms triggered by drug withdrawal.
The symptoms of comorbidities with substance use disorders are self-medicating tendencies, negative emotions, increased impulsivity, and reduced executive and cognitive functionality.
Comorbidities with substance use disorders are treated with medications and behavioral therapies. An integrated therapy regimen where both treatments are delivered concurrently has been found to be the most effective.
What does comorbidity with substance use disorders mean?
Comorbidity with substance use disorders (SUDs) means the presence of a SUD with another disorder or medical condition in the same person, at the same time or sequentially. Comorbidity implies the possibility that there is an interplay between the two disorders, with each ailment affecting the prognosis of the other. However, it is not always possible to establish causality or directionality in comorbid diseases. Comorbidities are typically chronic medical conditions.
What are the most common comorbidities with substance use disorders?
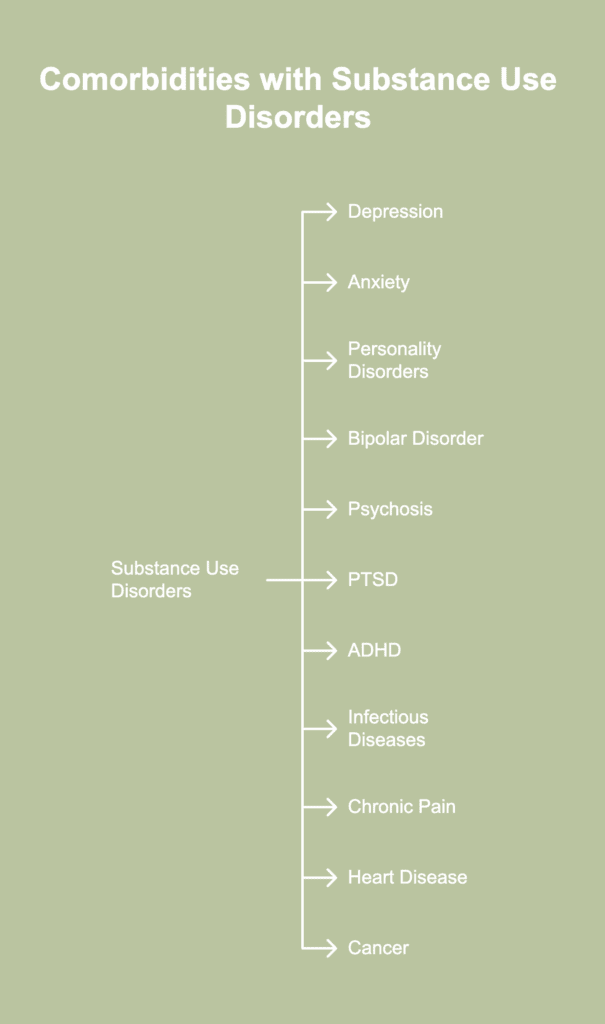
The most common comorbidities with substance use disorders are listed below.
- Depression: Comorbid major depressive disorder (MDD) in individuals with SUD is associated with poor quality of life, increased risk of disability, and greater risk of suicide, according to a 2012 article by Worley et al., published in the Journal of Substance Abuse Treatment, titled “Comorbid Depression and Substance Use Disorder: Longitudinal Associations Between Symptoms in a Controlled Trial.” It has been observed that MDD is the most prevalent mood disorder–with occurrence rates between 29.2% and 59.8%–in individuals with specific SUDs, according to the findings of a survey reported byCali A. Calarco and Mary Kay Lobo in the chapter titled “Depression and substance use disorders: Clinical comorbidity and shared neurobiology” from the 2021 edition of the International Review of Neurobiology.
- Anxiety: The rates of comorbid anxiety with SUDs are high, with 17.7% of individuals with a current SUD also diagnosed with anxiety, according to the findings of a survey reported in a 2008 article by Sudie E. Back and Kathleen T. Brady published in the journal Psychiatric Annals, titled “Anxiety Disorders with Comorbid Substance Use Disorders: Diagnostic and Treatment Considerations.” A diagnosis of anxiety includes panic and generalized anxiety disorders.
- Personality disorders (PD): The prevalence of personality disorders, typically antisocial PD and borderline PD, is high in individuals with a substance use disorder, with rates ranging between 34.8% and 73.0%, according to a 2018 article by Arpit Parmar and Gaurishanker Kaloiya published in the Indian Journal of Psychological Medicine, titled “Comorbidity of Personality Disorder among Substance Use Disorder Patients: A Narrative Review.”Comorbid PD is associated with very severe addiction problems and unfavorable treatment outcomes.
- Bipolar disorder: A comorbid diagnosis of bipolar disorder and SUD is prevalent in 30-60% of individuals with an addiction disorder, according to a 2022 article by Oliva et al., published in the Journal of Clinical Medicine, titled “Machine Learning Prediction of Comorbid Substance Use Disorders among People with Bipolar Disorder.” Individuals with bipolar disorder and a current SUD tend to have an earlier onset of disease, more instances of attempted and completed suicides, poor health outcomes, worse psychosocial functioning, and less treatment engagement, according to a 2011 article by Michael J. Ostacher published in the journal Focus, titled “Bipolar and Substance Use Disorder Comorbidity: Diagnostic and Treatment Considerations.”
- Psychosis: It has been observed that up to 70% of first episode psychosis patients have comorbid SUDs, according to a 2023 article by Rühl et al., published in the journal Frontiers in Psychology, titled “Remission with or without comorbid substance use disorders in early psychosis: long-term outcome in integrated care (ACCESS III study).” The substances most frequently implicated in this comorbidity are alcohol, tobacco, methamphetamines, and cannabis.
- Post-traumatic stress disorder (PTSD): On average, 30-50% of individuals seeking addiction treatment also fulfill the criteria for lifetime PTSD. A comorbid diagnosis of PTSD and SUD is associated with a more complex and expensive clinical course than having either mental illness alone.
- Attention-deficit/hyperactivity disorder (ADHD): The prevalence of ADHD was found to be 22% among individuals seeking treatment for SUD, according to a 2022 article by Effat et al., published in the journal Middle East Current Psychiatry, titled “Adult attention-deficit hyperactivity disorder among patients with substance use disorders.” Individuals with a comorbid diagnosis of ADHD and SUD tend to have a greater degree of cognitive impairment than those with ADHD alone.
- Infectious diseases: Injecting illegal drugs is a potent risk factor for developing infectious diseases like HIV (human immunodeficiency virus) and hepatitis A, B, and C, according to a 2020 article by Kolla et al., published in the Journal of Neurological Sciences, titled “Infectious diseases occurring in the context of substance use disorders: A concise review.” The use of illicit drugs, as well as alcohol, increases the risk of individuals developing bacterial and fungal infections.
- Chronic pain: Chronic pain is prevalent in 50-60% of individuals with SUD, according to a 2021 article by Wyse et al., published in the journal Pain, titled “Patients’ perceptions of the pathways linking chronic pain with problematic substance use.” The authors suggest that these two conditions are mutually reinforcing, share common neural circuits, and tend to be triggered by chronic stress.
- Heart disease: Individuals with SUDs are more likely to have an underlying cardiovascular disease (CVD) and develop incident CVD than those who do not have a SUD, according to a 2021 article by Gan et al., published in the journal Drug and Alcohol Dependence, titled “Risk of cardiovascular diseases in relation to substance use disorders.” Substances like alcohol, cocaine, and methamphetamine exert negative effects on the cardiovascular system, and their use is known to worsen disease progression in patients with heart failure.
- Cancer: Substance abuse increases the risk of developing cancer, especially in vulnerable individuals. On the other hand, patients with cancer are known to use drugs to manage cancer-related symptoms. SUD has been found to be most prevalent in survivors of head and neck cancer, esophageal and gastric cancer, cervical cancer, and melanoma, according to a 2024 article by Jones et al., published in the journal JAMA Oncology, titled “Substance Use Disorders Among US Adult Cancer Survivors.”
How common are comorbidities in substance use disorders?
Comorbidities in substance use disorders are very common, with 50-80% of individuals with SUD also having another mental health condition, as noted by the United Nations Office on Drugs and Crime in their 2022 paper titled “Comorbidities in Drug Use Disorders–No wrong door.”
The most common comorbidities in substance use disorders are panic disorder, social anxiety disorder, and antisocial personality disorder with their prevalence rates being 41.2%, 40.5%, and 39.3%, respectively, according to a 2023 article by Kar et al., published in the journal Scientific Reports, titled “Psychiatric comorbidities and concurrent substance use among people who inject drugs: a single-centre hospital-based study.”
On average, more than 60% of adolescents undergoing addiction treatment in community-based clinical settings are also diagnosed with a mental health disorder, according to a 2020 publication by the National Institutes on Drug Abuse (NIDA) titled “Common Comorbidities with Substance Use Disorders Research Report.”
What is the difference between dual diagnosis and comorbidity with substance use disorder?
The difference between dual diagnosis and comorbidity with substance use disorder stems from the nature of the diseases involved in the conditions. The differences are described in the table below.
| Dual diagnosis | Comorbidity with substance use disorder |
|---|---|
| Dual diagnosis is the simultaneous presence of a mental health disorder and a substance use disorder involving alcohol or drugs in the same individual. | Comorbidity with substance use disorder indicates the presence of another ailment, physical or mental, alongside the addiction issue in the same individual, simultaneously or sequentially. |
| It is a type of comorbidity with substance use disorder. | It is not a dual diagnosis if the condition occurring with the SUD is not a mental health disorder. |
| No physical ailment is involved in a dual diagnosis. | It is possible that comorbidity with substance use disorder involves physical disorders like chronic pain, heart disease, and cancer. |
Why do mental disorders and substance use disorders occur together?
Mental disorders and substance use disorders occur together primarily due to shared biological and environmental risk factors, the tendency of individuals to self-medicate the distressing symptoms of a mental disorder with substances, and drug-induced alterations in brain structure and functionality in regions also implicated in psychiatric conditions, according to a 2025 article by Ngo et al., published in the journal Complex Psychiatry, titled “Epigenetic Insights into Substance Use Disorder and Associated Psychiatric Conditions.”
However, it is challenging to establish directionality or causality in a comorbid diagnosis of mental disorder and SUD, according to a 2020 publication by the National Institutes on Drug Abuse (NIDA) titled “Common Comorbidities with Substance Use Disorders Research Report.” For instance, subclinical mental health disorders are known to cause individuals to initiate and maintain drug use in an attempt to self-medicate unpleasant symptoms.
On the other hand, it is not uncommon for individuals to fail to remember when they started using drugs, making it difficult to determine if the substance use problem or the mental illness occurred earlier.
What are the effects of comorbid conditions in substance use disorders?

The effects of comorbid conditions in substance use disorders are listed below.
- Increased severity of symptoms: Individuals who have comorbid mental health disorders with SUD tend to exhibit more persistent and severe symptoms than those with either disorder alone, according to a 2020 publication by the National Institutes on Drug Abuse (NIDA) titled “Common Comorbidities with Substance Use Disorders Research Report.” The symptoms tend to be resistant to treatment, thereby complicating the recovery journey.
- Drug-induced exacerbation of mental disorder symptoms: Drug abuse tends to exacerbate the symptoms of an underlying mental health disorder. For instance, drug dependence impairs the normal functionality of the neurotransmitter systems that the substance acts upon. An individual self-medicating their symptoms of depression or anxiety often feels more depressed and anxious because their brains have become dependent on drugs to feel “normal.”
- Withdrawal-induced aggravation of mental disorder symptoms: Drug withdrawal symptoms and those induced by a mental health disorder tend to overlap. This is especially applicable for rebound symptoms that tend to be more severe than what they were before the individual used drugs to self-medicate. It is critical that patients undergoing drug addiction treatment are monitored after a period of abstinence to distinguish between withdrawal symptoms and those induced by a psychiatric illness (NIDA, 2020)
- Poor treatment compliance: Individuals with comorbid mental health disorders and SUD tend to exhibit poor treatment adherence, resulting in poor clinical outcomes (NIDA, 2020). Furthermore, poor treatment adherence among patients with comorbid mental health illness with SUD is known to contribute to poor functioning across multiple areas of life, decreased quality of life, increased rates of hospitalization, and worse clinical outcomes compared to those who have a single disorder.
- Increased risk of overdose: The presence of comorbid psychiatric illnesses with SUD increases the risk of alcohol- and illicit drug-related overdoses. It has been found that 23.6% of all individuals who died of a substance overdose also had a depressive disorder, according to the findings of a study reported in a 2019 article by Iqbal et al., published in the journal Focus, titled “Treatment for Substance Use Disorder With Co-Occurring Mental Illness.”
- Increased suicidal behaviors: Comorbidity of SUD and other psychiatric illnesses is associated with an increase in suicidal behaviors like ideation, planning, attempts, and completed suicides. Suicidal behavior is highly prevalent in individuals with SUD alone. The presence of specific comorbid conditions like psychiatric disorders marked by anxiety or agitation, such as PTSD, and poor impulse control, such as conduct disorders, increases the risk of a suicide ideator moving to planning or attempting to take their lives, according to a 2011 article by Nock et al., published in the journal Molecular Psychiatry, titled “Mental Disorders, Comorbidity and Suicidal Behavior: Results from the National Comorbidity Survey Replication.”
What are the symptoms of comorbidities with substance use disorders?
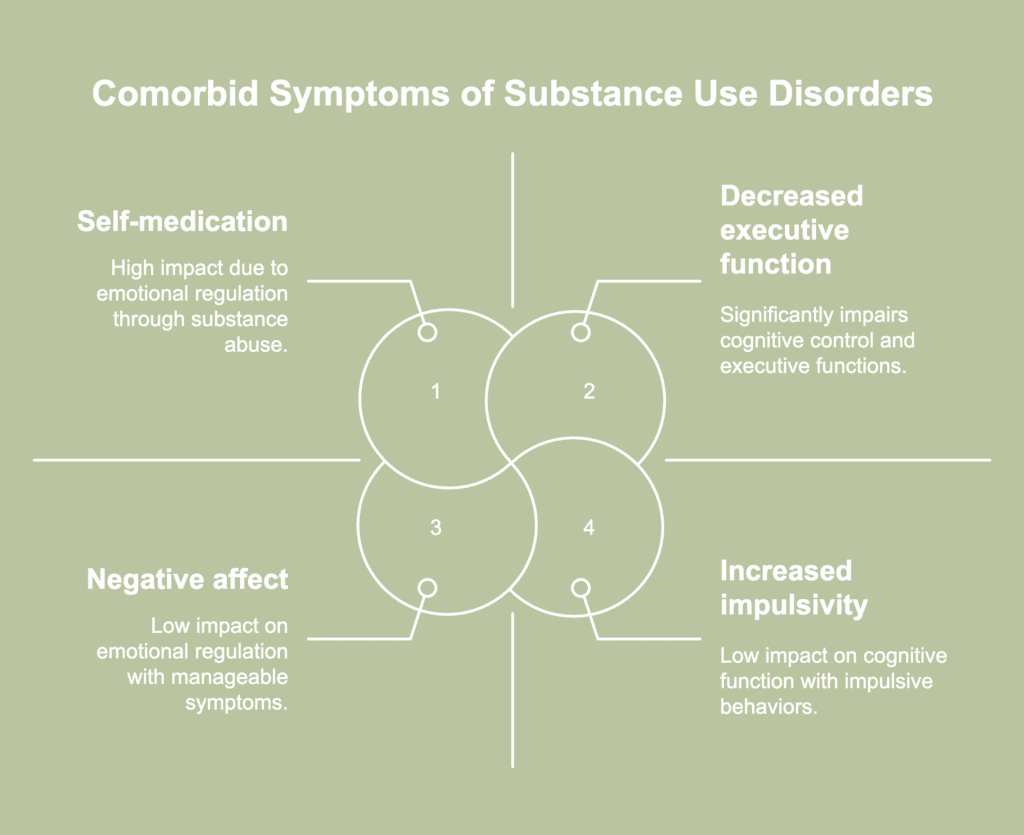
The symptoms of comorbidities with substance use disorders are listed below.
- Self-medication: Self-medication is an attempt by individuals with a mental health condition to address negative and painful emotional states by using substances of abuse. They feel overwhelmed by their emotions and use drugs to dampen them. Alternatively, a mental health disorder renders them unable to feel emotions, and they use substances to arouse themselves and experience “feelings.”
- Negative affect: Negative affect is marked by feelings of sadness, depression, anxiety, stress, guilt, and shame. It is a common shared feature between SUDs and other psychiatric disorders, according to a 2024 article by Wormington et al., published in the journal Psychiatry Research, titled “The genetic architecture of substance use and its diverse correlations with mental health traits.”
- Increased impulsivity: The DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, 5th edition) notes that impulsivity is a common cognitive issue associated most frequently with SUDs and other psychiatric illnesses like disruptive, impulse-control and conduct disorders, and ADHD, according to a 2024 article by Zharia C. Crisp and Jon E. Grant published in the journal Comprehensive Psychiatry, titled “Impulsivity across psychiatric disorders in young adults.” Impulsivity manifests as behavioral traits like decreased inhibitory control, failure to resist urges and delayed gratification, inability to plan and adhere to long-term goals, and being unable to foresee or having no regard for potential risks or negative consequences. These traits are associated with regions in the brain, such as the thalamus, cortex, and striatum, that are implicated in SUDs and other mental illnesses.
- Decreased executive function: Decreased executive functionality is associated with mental health conditions like schizophrenia, bipolar disorder, depression, and obsessive-compulsive disorder. Executive functionality includes the cognitive mechanisms required for regulating behavior, emotions, and attention. Drugs of abuse are known to impair the functionality of the prefrontal cortex region that influences cognitive control and executive functions.Impairment of cognitive control is both a cause and a consequence of mental health disorders, including SUDs.
What are the risk factors for comorbidities with substance use disorders?
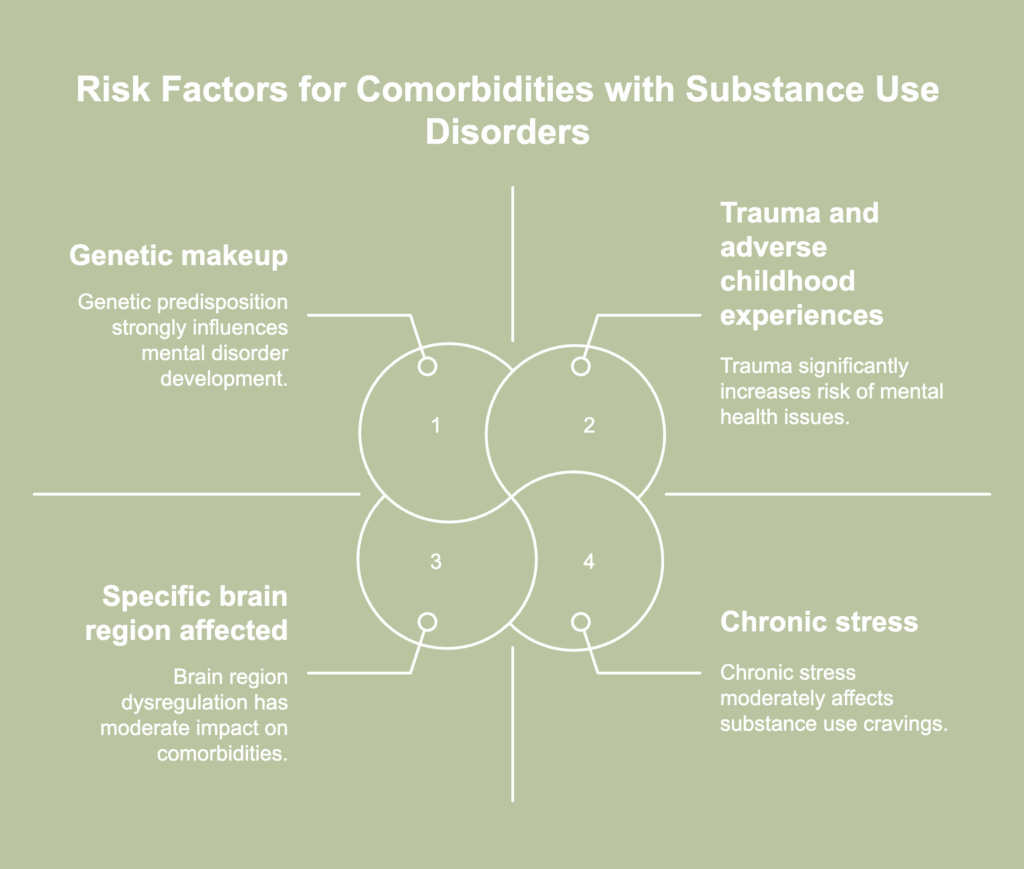
The risk factors for comorbidities with substance use disorders are listed below.
- Genetic makeup: Genes influence how an individual responds to stress or whether they tend to engage in novelty- or thrill-seeking behaviors. Thus, genetic predisposition is attributable to the development of mental disorders as reactions to stress and the initiation and exacerbation of SUDs, according to a 2020 publication by the National Institutes on Drug Abuse (NIDA) titled “Common Comorbidities with Substance Use Disorders Research Report.” For instance, specific genes influence the actions of neurotransmitters like dopamine and serotonin. Dysregulation of their functionalities is implicated in the development of both mental disorders and SUDs. Studies on behavioral genetics suggest that shared genetic factors influence externalizing behaviors and vulnerability to SUD, according to a 2024 article by Wormington et al., published in the journal Psychiatry Research, titled “The genetic architecture of substance use and its diverse correlations with mental health traits.”
- Epigenetic influences: Epigenetics refers to alterations in gene functionality that are not caused by changes in the underlying DNA sequence but are due to the influence of environmental factors like trauma, chronic stress, or drug exposure. Mental disorders and SUDs are not disparate entities but have been found to co-occur because they share epigenetic mechanisms. Alcohol and illicit drug abuse induce neurobiological adaptations within the genes involved in neurotransmitter regulation, stress response, reward processing, and emotion regulation that are also implicated in psychiatric conditions like schizophrenia, stress, anxiety, and depression, according to a 2025 article by Ngo et al., published in the journal Complex Psychiatry, titled “Epigenetic Insights into Substance Use Disorder and Associated Psychiatric Conditions.” Epigenetic alterations are also possible due to prenatal and/or early-life exposure to maternal stress, malnutrition, and toxins; childhood trauma; and environmental pollutants. Specific epigenetic changes are heritable, meaning that they are passed down through generations in a family, thereby influencing the vulnerability of future generations to developing mental illness and SUD.
- The specific brain region affected: Regions in the brain associated with reward processing, emotion regulation, decision making, and impulse control, and neurotransmitter systems like dopamine, serotonin, GABA (gamma-aminobutyric acid), and glutamate are implicated in both substance abuse and mental health disorders like depression and schizophrenia. Dysregulation in these systems and areas caused by one disorder is likely to precipitate the onset of the other (NIDA, 2020).
- Chronic stress: Mental stress and negative emotional states induce cravings in individuals dependent on a substance of abuse, according to a 2005 article by Kathleen T. Brady and Rajita Sinha published in The American Journal of Psychiatry, titled “Co-Occurring Mental and Substance Use Disorders: The Neurobiological Effects of Chronic Stress.” Chronic stress deregulates the hypothalamic-pituitary-adrenal (HPA) axis and impairs dopamine signalling, thereby increasing the reinforcing effects of drugs. Dysregulation of the HPA axis impairs normal functionality in the brain regions associated with motivation, learning, and adaptation. Dysfunctionality of these regions is implicated in substance abuse (NIDA, 2020). Additionally, drug use impairs the stress response system by altering critical neurotransmitter functionality.
- Trauma and adverse childhood experiences: Scientific evidence proves the link between the trauma of adverse childhood experiences (ACEs) and poor mental health outcomes. Individuals who have experienced ACEs have an increased risk of developing mental health problems like SUD, depression, and bipolar disorder, according to a 2023 article by Tzouvara et al., published in the journal Child Abuse & Neglect, titled “Adverse childhood experiences, mental health, and social functioning: A scoping review of the literature.” Trauma alters biological systems, such as reducing the volume of the prefrontal cortex, which causes an individual to behave impulsively and engage in risky drug-use behaviors. Trauma hyperactivates the HPA axis, resulting in an overactive stress response system, which is a significant factor in developing PTSD. It is likely that individuals abuse substances to self-medicate symptoms like anxiety triggered by PTSD and/or distract themselves from their trauma (NIDA, 2020).
- Presence of a mental disorder: Robust scientific evidence suggests that there is a significant association between the presence of all mental disorders and the onset of drug use, the transition from intermittent use to abuse and that from abuse to dependence, according to a 2011 article by Swendsen et al., published in the journal Addiction, titled “Mental Disorders as Risk factors for Substance Use, Abuse and Dependence: Results from the 10-year Follow-up of the National Comorbidity Survey.” The association is the strongest and the most consistent for behavioral disorders and another SUD. The greater the number of mental disorder diagnoses, the greater the risk of the onset of each stage of substance use. The reasons include a tendency to self-medicate symptoms of the mental illness with substances of abuse, as well as specific disease-induced neurobiological changes that increase the vulnerability of the individual for developing SUD (NIDA, 2020).
- Presence of a SUD: Drug abuse causes structural and functional alterations in brain regions that are implicated in mental illnesses like anxiety, schizophrenia, and mood- and impulse-control disorders. In individuals with a genetic vulnerability to a mental disorder, drug use is known to trigger the onset of the disease (NIDA, 2020).
How are comorbidities with substance use disorders diagnosed?
Comorbidities with substance use disorders are diagnosed using a comprehensive approach that includes behavioral observations, clinical interviews, and screening tools. Commonly used standardized and validated screening tests to diagnose problematic alcohol and drug use patterns include questionnaires like the Drug Abuse Screen Test (DAST or DAST-10), Tobacco, Alcohol, Prescription medication, and other Substance use (TAPS), Cut-down Annoyed, Guilty, Eye-opener (CAGE), CAGE-AID (Cut-down, Annoyed, Guilty, Eye-opener-Adapted to Include Drug use), and Car, Relax, Alone, Forget, Friends, Trouble (CRAFFT), the latter being a test customized for teenagers. The DAST-20 is a screening tool customized for adolescents. Physical examinations that include laboratory blood and urine tests are used to confirm a diagnosis of SUD during the assessment process.
Psychiatric or psychological evaluations are made by professional healthcare practitioners as part of the diagnostic protocol. Psychiatric disorders are diagnosed by licensed psychologists using structured clinical interviews that aim to gather information about the patient’s disease history, experiences, and symptoms. Individuals who enter substance abuse treatment continue to be observed after a period of abstinence to distinguish between symptoms of intoxication or withdrawal and those associated with a comorbid psychiatric disorder.
How are comorbidities with substance use disorders treated?

Comorbidities with substance use disorders are treated with medications and behavioral therapies like cognitive behavioral therapy, dialectical behavior therapy, contingency management or motivational incentives, exposure therapy, assertive community treatment, therapeutic communities, and integrated group therapy, according to to a 2020 publication by the National Institutes on Drug Abuse (NIDA) titled “Common Comorbidities with Substance Use Disorders Research Report.” Adolescents and young adults who develop substance use and other mental health disorders tend to have an increased risk for severe psychiatric problems later in life.
Therapies like multisystemic theory, multidimensional family therapy, and brief strategic family therapy are tailored to the unique needs of adolescents and children with comorbid mental health disorders with SUD. These therapies have been shown to be effective in managing their condition when delivered alongside medications and other forms of behavioral counseling. It is believed that medications like bupropion that are approved for treating nicotine dependence and depression have the potential to be effective in managing comorbid mental health disorders and SUD.
Clozapine is effective in treating problematic alcohol, cocaine, and cannabis use in patients with schizophrenia, according to a 2013 article by Kelly et al., published in the journal Addictive Behaviors, titled “Treatment of Substance Abusing Patients with Comorbid Psychiatric Disorders.” It is challenging for individuals with comorbid mental health conditions with SUD to find homes with healthy environments, earn a sustainable livelihood, and/or navigate life’s routine chores, resulting in additional mental stress. Directing these patients to appropriate social support services that help them reorganize their lives promotes treatment success and helps them achieve their goals.
Substance use causes epigenetic alterations in brain areas associated with multiple psychotic illnesses, resulting in increased severity of symptoms. On the other hand, the presence of a mental health disorder is known to trigger the transition from intermittent and controlled drug use to uncontrolled and compulsive substance use and also contribute to the maintenance of addiction by increasing the risk of relapse. An integrated therapeutic protocol that aims to treat both disorders concurrently has been found to consistently deliver superior clinical outcomes than addiction treatment and mental health therapy administered separately, according to a 2013 article by Thomas M. Kelly and Dennis C. Daley published in the journal Social Work in Public Health, titled “Integrated Treatment of Substance Use and Psychiatric Disorders.” Severe comorbid psychiatric conditions have been found to benefit from highly structured treatment regimes that combine intensive outpatient therapy, behavioral therapies, and case management services (Kelly et al., 2013).
Why is it important to address comorbidities with substance use disorders?
It is important to address comorbidities with substance use disorders because the persistence of each disorder tends to exacerbate the symptoms of the other. The interplay between the two diseases makes treating the patient more complicated and significantly diminishes the chances of positive clinical outcomes compared to when an individual has either disorder alone. If left untreated, individuals with comorbid mental health conditions with SUD experience a more chronic and treatment-resistant course that impairs multiple areas of their lives, ranging from their mental well-being and physical health to interpersonal relationships, employability, and professional progress.
Addressing comorbidities with substance use disorders leads to improved treatment outcomes, reduced risk of addiction relapses, lower healthcare expenses stemming from a diminished risk of contracting infections and reduced hospitalization rates. In addition, there is improved quality of living, enhanced psychosocial functioning, with greater chances of social reintegration.


